Rachel Zoffness Ph.D.
Is It Possible to Change Pain?
The science behind why pain is painful.
Posted Nov 21, 2019
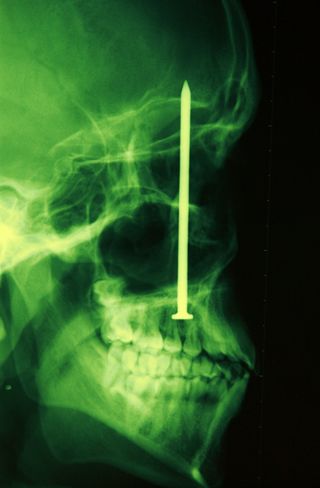
You may be in pain, but this man has a nail in his head.Source: Denver Post file photo, used with permission.
You may believe that pain is a purely biological process that has nothing to do with your thoughts, perceptions or emotions. This would be reasonable, given that Western medicine has incorrectly – and dangerously – divided humans into two disconnected entities: mind (“mental”) and body (“physical”).
But when it comes to pain, this divide couldn’t be less helpful – or more wrong.article continues after advertisement
Thoughts, beliefs, perceptions, emotions, past experiences, context, and input from your body all affect your experience of pain (Edwards et al, 2016). All of the time, always. To demonstrate this point, I present to you: A Tale of Two Nails. Sit down for this one, friends.
In 1995, the British Medical Journal reported that a 29-year-old construction worker had suffered an accident: after jumping onto a plank, a 7-inch nail had pierced his boot clear through to the other side (Fisher et al, 1995). In terrible pain, he was carted off to the ER and sedated with opioids. When the doctors removed his boot, they discovered a miracle: the nail had passed between his toes without penetrating his skin! There was zero damage to his foot: no blood, no puncture wound… not even a scratch. But make no mistake: despite the absence of injury, his pain was real. So what happened?
Sensory receptors in the man’s body reported to his brain that there’d been an accident, that a nail had penetrated his boot. His brain, perceiving potential threat to his safety and well-being, used context to determine what had occurred, collecting information from his five senses (including the visual of a nail sticking out of his shoe!), knowledge of the dangerous work environment and its risks, his co-workers’ horrified faces, and other data to make a guesstimate about what had happened and how to respond. Thoughts, beliefs and emotions – including panic and fear – set off a cascade of biological and neurochemical processes. His brain, synthesizing the sum total of this information, decided that he was in danger, so it made pain to protect him. In this case, real pain was generated entirely as a result of factors having nothing to do with actual tissue damage – yet was as intense as if he’d been stabbed.
On the flip side, another construction worker (dangerous job, that!) was using a nail gun when it unexpectedly discharged, clocking him in the face (Dimsdale & Dantzer, 2007). Other than a mild toothache and a bruise under his jaw, he thought he’d escaped unscathed. Six days later – six days of eating, sleeping, and going to work – he went to the dentist. Much to his surprise, an X-ray revealed a 4-inch nail embedded in his head! Because contextual cues failed to put his brain on high-alert, his pain system remained quiet – despite actual bodily harm and need for medical intervention (#fail).
These Tails of Nails highlight a number of important points (pun intended!) for pain-sufferers and health providers. The first is that pain is not an accurate indicator of tissue damage. You can experience terrible pain in the complete absence of bodily harm (e.g., a nail in the shoe but not the foot), and little pain in the presence of significant damage (e.g. a nail to the face!). That is: just because something hurts does not necessarily mean your body is in danger of harm. “Hurt” and “harm” are not the same.article continues after advertisement
The second takeaway is that thoughts, perceptions, emotions, and context – in addition to sensory inputs from the body – define the human experience of pain, both amplifying and reducing it (Gatchel et al, 2007; Turk et al, 2016). You’ve likely experienced this phenomenon many times. For example, have you ever played a soccer game that was so much fun you didn’t realize your leg was bleeding until after the game was over? Or discovered mysterious black-and-blue marks, having no idea how they got there…? Similarly, potentially painful stimuli – like a bite or slap – can feel good during sex and painful in other contexts. This is because cognitive, emotional and contextual factors like excitement, distraction, pleasure, and attentional processes constantly regulate your experience of pain.
Dr. Henry Beecher, a war-time anesthesiologist, reported a similar phenomenon in a 1946 article about wounded soldiers. He noticed that the extent of soldiers’ injuries didn’t correlate with the degree of pain they experienced. In fact, 75% of the severely wounded soldiers – now safe from battle with the comforting possibility of going home – reported little to no pain despite having serious injuries. In the words of the esteemed doctor: “There is a common beliefthat wounds are inevitably associated with pain, and, further, that the more extensive the wound, the worse the pain” (Beecher, 1946). This, he observed, was not true.
What we now know is that pain is a guesstimate: your brain’s best guess as to whether your body requires protection, and how much. Context – the sum total of all available information from your internal and external environments – is critically important to pain processing, and always informs your experience of pain. That is: pain is never purely biological, due exclusively to issues like tissue damage and anatomical dysfunction. It is also emotional, social and cognitive, constantly influenced by thoughts, perceptions, emotions, and context (Bushnell et al, 2013; Gatchel et al, 2007).article continues after advertisement
The take-home messages from these cautionary Tales of Nails:
(1) Pain is not “all in your head.” However, it IS – at least in part – in your brain.
(2) Pain is not an accurate indicator of tissue damage. “Hurt” and “harm” are not the same.
(3) Cognitive, emotional and contextual factors always inform pain processing. Specifically, credible evidence that your body is in danger can amplify pain, while credible evidence of safety can reduce pain (Butler & Moseley, 2013). Changing thoughts, perceptions, and emotions – what you think, how you feel, and what you believe about your body and your health – can, therefore, change the pain you feel. This means that you have more control over your pain than you may have realized.
(4) Treating chronic pain with exclusively biomedical solutions like pills and procedures is insufficient. This limited treatment approach is one of the primary causes of the opioid epidemic, and has been shown to be ineffective for long-term care (NIH, 2019; USDHHS, 2019a).
(5) Effective pain treatment requires addressing biological, psychological and social components of pain. This may be achieved by adding Cognitive Behavioral Therapy (CBT), biofeedback, Mindfulness-Based StressReduction (MBSR), graded exercise, and other non-drug, non-surgical interventions to the treatment plan (Kerns et al, 2011; Majeed & Sudak, 2017), or going to an integrative pain management clinic. Going to therapy for pain does not mean you’re “crazy.” Biobehavioral approaches like these are low-risk, have evidence of effectiveness (Garland et al, 2019), have no side effects, and are now considered best practice in pain medicine (USDHHS, 2019b). You literally have nothing to lose!
And the final tip, which may be last, but certainly isn’t least:
(6) Never shoot yourself in the face with a nail gun.
… You may not even notice.
References: To view a list of the references used in this article, go to the “Link to the Original Article” listed below.
About the author: https://www.psychologytoday.com/ca/experts/rachel-zoffness-phd
Link to original article: https://www.psychologytoday.com/ca/blog/pain-explained/201911/is-it-possible-change-pain
Tags: long-term care, biomedical solutions, Cognitive, emotional, contextual, guesstimate, biological, tissue damage, anatomical dysfunction, emotional, social, cognitive, constantly, thoughts, perceptions, emotions, context


